Our innovation is inspired by patients
At Ionis, our efforts begin and end with the patient in mind. From discovery to development to getting medicines into the hands of those who need it, we are inspired by the needs of the patient communities we serve, and fueled by the promise of our science. Every aspect of what we do is grounded in patient perspectives.
Take a closer look at some of the people who inspire our work.
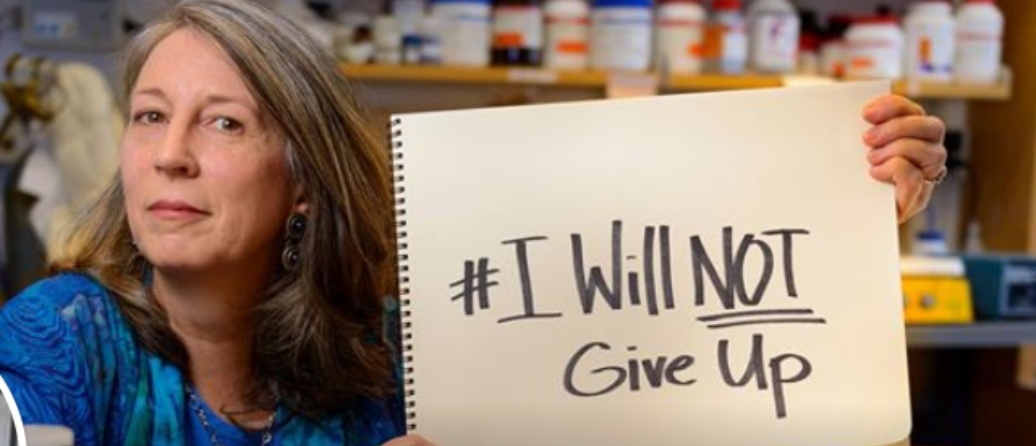
Lou and Terry Jo’s story
When her son Louie (Lou) was born, Terry Jo already had four daughters, including a set of identical twins. As a nurse-midwife, she learned while working in Nigeria, where more twins are born than in any other country, that the child born after twins carries big luck. So, she and her husband thought they would try for a boy and were thrilled when he was born. Little did they know their lucky baby had something unlucky lurking in every neuron in his brain.
See More »Lou and Terry Jo’s story
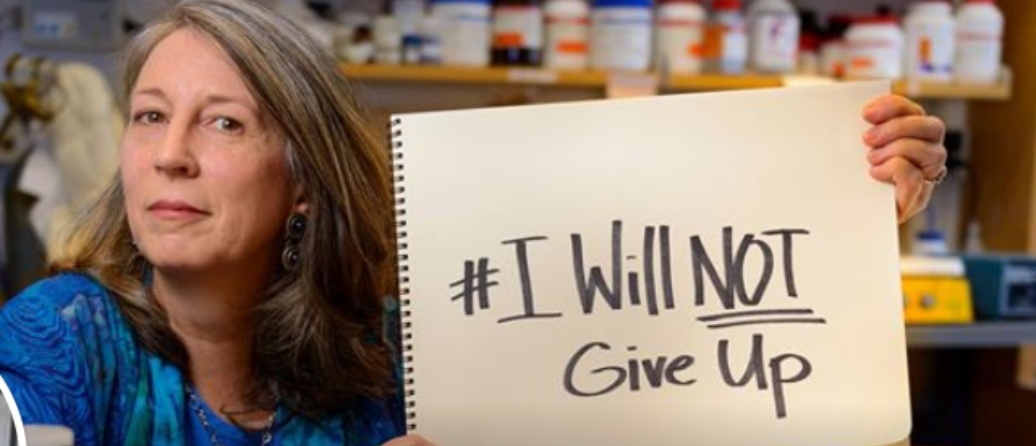
An elusive diagnosis
When her son Louie (Lou) was born, Terry Jo already had four daughters, including a set of identical twins. As a nurse-midwife, she learned while working in Nigeria, where more twins are born than in any other country, that the child born after twins carries big luck. So, she and her husband thought they would try for a boy and were thrilled when he was born. Little did they know their lucky baby had something unlucky lurking in every neuron in his brain.
Lou was a cuddly and adorable baby, but his mother sensed he was different from her other children. When he turned one year old and was still unable to sit up or crawl, a neurologist diagnosed him with cerebral palsy. With a diagnosis that did not seem right, Terry Jo and her husband, Dave, flipped through medical text books, stumbling upon a page about Angelman syndrome (AS). Lou looked a lot like the people in the photos, but it was hard to believe that he was severely cognitively disabled.
The family made an appointment with Dr. Ken Lyons Jones, who happened to be the author of their medical textbook. He looked at cheerful little Lou, who was not meeting his milestones, had a tremulousness about his movements, and he took his tuning fork and placed it on Lou’s knee. Lou laughed hysterically—one of the hallmark symptoms of AS. After a blood test, the diagnosis was confirmed.
People with AS are unable to speak and are dependent on others 24 hours a day. Many have intractable seizures and are unable to sleep. It is an incurable, rare disease, and a devastating diagnosis.

A tireless search for answers
Dissatisfied with the lack of treatment options for AS, Terry Jo and Dave scoured scientific and medical literature written about AS, determined to become experts in UBE3A, the maternal gene that Lou was missing. UBE3A is a ubiquitin ligase, which targets
proteins for destruction in the cellular recycling center. Terry Jo and Dave learned that Lou was missing UBE3A in every neuron in his brain, which meant that Lou would remain unable to speak, unable to sleep, and possibly unable to walk or feed himself for the rest of his life. Feeling helpless, Terry Jo booked a flight for her and Lou to attend the first international AS meeting in Finland.
During her travels, she met Dr. Arthur Beaudet, a geneticist, who had discovered the gene for AS. He firmly believed it to be a curable disorder since AS occurs when there’s a problem on the mother’s chromosome while the paternal gene is perfectly fine, it’s just silenced. Dr. Beaudet believed it possible to unsilence the paternal gene.
With this news, Terry Jo, impatient for any progress in the field, went back to school to get a PhD in neuroscience determined to discover a compound that could unsilence the paternal gene. As she continued to work on as many experiments and studies as she could in graduate school, the field started to get a lot of attention.
Everything for Terry Jo changed when a young scientist at the University of North Carolina, Ben Philpot, completed the experiment that she had hoped to do. He looked at thousands of compounds and found that a cancer drug, topotecan, could unsilence the paternal gene.
Their moment of YES
Dr. Beaudet suggested Terry Jo get in touch with Ionis, who believed the company’s antisense technology could help her achieve the goal of disrupting the defective, or silenced chromosome. Positive about pursuing change for the AS community, Ionis welcomed families, representatives from foundations, and reviewed notebooks full of letters from all over the world expressing a strong desire for a genetic treatment, despite the fact that the greater AS community was still debating whether or not a cure was possible.
Today, Ionis hopes to begin clinical trials in patients in the near future for a treatment thought to help those with AS, instilling new hope for a brighter future.
To this day, Terry Jo believes in the power of information. Because she never stopped seeking answers for Lou, she found Ionis, which may hold the key to a new tomorrow for those with AS.

Fred and Lynne’s story
Fred and Lynne have been married for 40+ years. When talking about Fred’s illness, Lynne often looks back to when she said, “I do,” and thinks about how she had no idea at the time what “in sickness and in health” would really mean.
See More »Fred and Lynne’s story

A mysterious condition
Fred and Lynne have been married for 40+ years. When talking about Fred’s illness, Lynne often looks back to when she said, “I do,” and thinks about how she had no idea at the time what “in sickness and in health” would really mean.
During their third year of marriage, Fred learned that his brother was diagnosed with cancer, as well as a rare condition. Since the condition was hereditary, Fred was also tested. Although he had no symptoms, he tested positive for what at the time was
considered hyperlipidemia, which today is known as familial chylomicronemia syndrome (FCS).
FCS occurs in about one in one million people and is a genetic disorder in which the body cannot break down certain fats correctly. This disease frequently leads to symptoms such as pancreatitis, a very serious condition that causes inflammation of the pancreas and can lead to death, and fatty deposits in the skin. With no treatment available at the time of diagnosis, Fred was told to modify his lifestyle to keep his triglycerides down.
At first, incorporating these changes seemed relatively minor. Lynne and Fred switched to a low-fat diet, he tried to exercise more, and life continued as a young married couple. Fred felt good and pursued a career as a research chemist for about 20 years.
But in the late ’90s, things began to change. Subtle at first, his triglycerides rose from 200 to 500, even though his diet and
exercise regimen remained the same. His doctor placed him on medication in hopes of lowering his triglycerides, but they
continued to rise, going as high as 8000. A diagnosis of type II diabetes at this same time did not help.
An isolating journey
As the year 2000 approached and the world was speculating about what the new century would bring, Lynne and Fred didn’t
anticipate how much their own world would change. Like so many who suffer from FCS, Fred’s medical journey started to become an odyssey. Feeling discouraged and helpless, their search for answers began.
The sense of hopelessness Fred felt was contagious. Lynne did her best to be strong. Being a Registered Nurse helped her be his advocate since she understood the doctors and was able to translate it in a way both she and Fred could comprehend. Throughout their journey to grasp why this was happening, Fred experienced frequent episodes of pancreatitis, with abdominal pain, vomiting and diarrhea, and mental fog. As a result, Fred required a lot of down time. He continued to work as a chemist during the week, but the weekends he spent in bed, trying to regain strength and stamina for the week ahead. Being home was safe, yet isolating.
In 2015, Fred was officially diagnosed with familial chylomicronemia syndrome (FCS), three words the couple explains as being hard to pronounce, yet a relief to hear. After all those years of searching and hoping, the fact that Fred’s rare disease actually had a name legitimized his experience to the world.
Their moment of YES
The couple soon learned about a clinical trial for those with FCS, studying volanesorsen, a potential treatment designed to reduce the production of a protein produced in the liver that plays a central role in the regulation of plasma triglycerides and may also affect other metabolic parameters. Ionis believes its antisense technology could disrupt the production of this protein. After so many years of battling an unknown, debilitating disease, this news felt life-affirming on many levels.
Since the trial ended, Fred still has bad days, but recently, his good days outnumber the bad. Through this experience, the couple also found an FCS community and share their experiences. With the good days becoming more frequent and a support system in place, Fred and Lynne remain hopeful for their future.

Sonia and Eric’s story
In 2010, otherwise healthy mother and poet Kamni Vallabh started to experience weakened eye sight. Kamni’s journey that started as a few visits to the ophthalmologist soon escalated into a dizzying array of specialists as both her mental and physical decline progressed. Testing Kamni for everything under the sun, from heavy-metal poisoning to Lyme disease, meant only one thing was for sure—Kamni’s illness was unknown.
See More »Sonia and Eric’s story

An unknown illness
In 2010, otherwise healthy mother and poet Kamni Vallabh started to experience weakened eye sight. Kamni’s journey that started as a few visits to the ophthalmologist soon escalated into a dizzying array of specialists as both her mental and physical decline progressed. Testing Kamni for everything under the sun, from heavy-metal poisoning to Lyme disease, meant only one thing was for sure—Kamni’s illness was unknown.
Finally, in December 2010, Kamni’s family received the diagnosis that had been elusive for so long—prion disease. Prion disease occurs when normal prion proteins, found on the surface of many cells, become abnormal and clump in the brain, causing memory problems, personality changes, and trouble with movement—many of the same symptoms that plagued Kamni as the prions
aggressively made their way through her brain tissue, causing irreparable damage.
Since prion disease is currently incurable, this diagnosis didn’t bring relief for the family, and Kamni passed away in late 2010.
Taking action in the face of uncertainty
An autopsy revealed that Kamni’s prion disease was a genetic subtype sometimes called fatal familial insomnia (FFI), and through predictive testing, the family learned that Kamni’s daughter, Sonia, would eventually succumb to the disease that took her mother’s life. Prion diseases are extremely rare. Between all of the different subtypes, which include Creutzfeldt-Jakob disease (CJD) and Gerstmann-Straussler-Scheinker disease (GSS) in addition to FFI, only about 300 cases are reported in the US each year.
This news sparked a new life pursuit for Sonia and her husband, Eric. Although Eric had recently completed his master’s degree in Urban Planning at MIT and Sonia had graduated from Harvard Law School, they both eventually quit their jobs to focus on finding a cure full time. For the next few years, refusing to sit back and let the disease ravage her family, the couple was determined to live and breathe the science of the disease. But as the couple got deeper in research, the gravity of their challenge began to sink in. Hope they originally felt while unearthing preliminary research crumbled as limitations of possible treatment approaches became evident, due in part to the challenge of identifying a strategy that could stop brain damage before it’s too late.
Their moment of YES
During this time, the couple met Jeff Carroll, a scientist who partnered with Ionis to develop a therapy for Huntington's Disease, a disease with which he had been diagnosed. Similar to Jeff’s work with Ionis, Sonia and Eric learned that Ionis’ antisense technology may also help make a positive difference in the lives of those with prion disease. And, Ionis said yes and stepped in to help.
Ultimately, with Ionis’ help, Sonia and Eric were cleared by the FDA to develop a therapy for prion disease.
The next big challenge is for the couple to recruit people at risk for genetic prion disease to the natural history study they are helping to run at Massachusetts General Hospital. With a disease so rare, recruitment may be a challenge. But with renewed hope and purpose, there’s no telling how far their pursuit will go.

Chuck’s story
In Chuck’s family, the awareness of hATTR amyloidosis started with his uncle Bill, who was on a mission to find out what was wrong with him. He called an Amyloidosis Center of Excellence, gave them his symptoms, and within a week saw a doctor who diagnosed him.
See More »Chuck’s story

A family diagnosis
In Chuck’s family, the awareness of hATTR amyloidosis started with his uncle Bill, who was on a mission to find out what was wrong with him. He called an Amyloidosis Center of Excellence, gave them his symptoms, and within a week saw a doctor who diagnosed him.
But the diagnosis did not stop there as Bill suspected others in the family should be tested as well. Bill's sister, who is Chuck's mom, was the next one who received a positive diagnosis. After his mother was diagnosed, Chuck went for testing and found out he was also positive for hATTR.
Out of 24 family members who were tested, 18 are positive—including two out of Chuck’s three sons and his two remaining siblings.
Hereditary ATTR amyloidosis (hATTR) is an inherited disease that often affects the liver, nerves, heart and kidneys. The disease is characterized by the deposit of an abnormal protein called amyloid in multiple organs of the body where it should not be, which causes disruption of organ tissue structure and function. The amyloid deposits most often occur in tissues of the nervous system, heart, and digestive tract.
Chuck’s first symptoms were autonomic issues, such as nausea, vomiting and diarrhea, and he thought it was just part of getting older. But as he became more symptomatic, hATTR started to completely change his life.
A rare disease that robs its patients
Later, he developed additional polyneuropathy symptoms, such as pain in his hands and feet, loss of grip and dexterity in his hands, balance issues, stumbling and falling and tingling and numbness in his hands and feet. These symptoms got so bad he felt like he could not carry his grandchildren.
Active throughout his life, he enjoyed riding his bicycle, dancing, and racing motorcycles. But hATTR robbed him of what he loved.
His moment of YES
Chuck was just about to give up when someone from his support group told him to go to a meeting about Ionis' NEURO-TTR clinical trial, which was designed to study the safety and efficacy of inotersen from Ionis. Inotersen is an antisense drug that was designed to decrease the amount of mutant and normal TTR made by the liver. Ionis believed that decreasing the amount of TTR protein would result in a decrease in the formation of TTR deposits, and thus slow or stop disease progression. Chuck met the criteria for the trial and began participation, and was excited at the potential to help those living with hATTR.
Since the trial’s completion and subsequent FDA approval, inotersen, now known as TEGSEDI™ has become available to treat patients like Chuck. With optimism for the future for himself and his sons, Chuck’s advice to anyone living with this disease is to face it with strength, and to be thankful that hope has been renewed for those living with hATTR.

